The infections caused by the Candida fungus are opportunistic. It is necessary that there’ll be alterations in the defenses of the organism so that they occur.
Candidiasis are mycoses, infections produced by fungi belonging to the Candida species.
- They may be acute, or chronic infections.
- They affect the skin, mucous membranes and deep tissues.
- The symptoms are very variable.
- The prognosis is also very variable. From muco-cutaneous light infections to the life of the patient compromised in cases of severe immunosuppression.
- These are opportunistic mycoses.
It is a type formed by fungus with the appearance of yeast, mostly unicellular. Within the type, the species of clinical interest are:
- Candida albicans: it is the most virulent species and responsible for more than half of the cases.
- Candida glabrata
- Candida parapsilosis: associated with the use of catheters, probes and needles.
- Candida krusei: associated with taking Flukonazole (it is an antifungal)
different types of candidiasis
What are the opportunistic pathogens?
Opportunistic pathogens are those that, under normal conditions, do not infect a healthy person. There must be an alteration in one of the biological barriers of the immune system for this to happen.
The Candida type, like the majority of fungus and some bacteria, belong to this group of pathogenic elements. In fact, Candida is part of the normal flora of the skin and mucous membranes in a large percentage of the population.
How does candidiasis occur?
By the alteration of mechanical barriers: damage to the skin and the mucous membranes (primary barriers)
This is what happens in patients with catheters, probes, prostheses or dialysis. This also explains the infection of drug users by parenteral (injectable) drugs.
If the fungus passes through the bloodstream, this can affect any organ. It appears in patients with severe immunosuppression (poorly controlled and terminally ill HIV).
Damage to the skin or mucous membranes prevents this zone from acting as a barrier and allows colonization by the fungus. This is why syringe bites or erosion of the mucosa caused by a catheter predispose to infection.
Due to alterations in the bacterial flora
Damage to the bacterial flora often occurs because of the use of broad-spectrum antibiotics. This is due to their very broad scope. Antibiotics “attack” both the bacteria responsible for infection and those that are part of the flora. At the moment when this barrier disappears, mycosis is made possible.
For example, it is relatively common to find cases of vaginal candidiasis in young women after taking antibiotics.
Immunodepression states
They may be caused by a disease, as is the case with HIV patients, or may be of pharmacological origin, as is the case in patients transplanted and treated with anti-rejection drugs.
how can you diagnose a candidiasis?
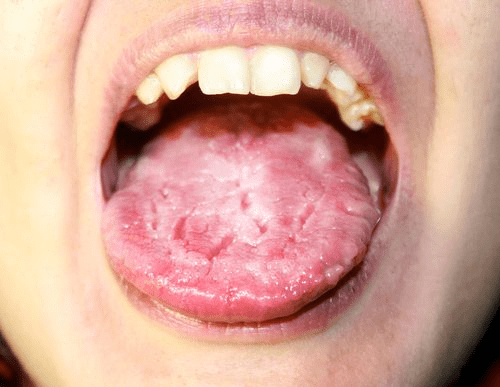
Muguet (oropharyngeal candidiasis)
It is characterized by the appearance of white pseudomembranes that cover the tongue, the soft palate and the oral mucosa. If they are removed, they reveal a red and worn surface. They can become very painful and compromise swallowing and breathing.
It appears mostly in HIV-infected patients (up to 90%), as it is one of the first manifestations of the disease. Although this is one of the most frequent opportunistic infections that affect these patients, the incidence has recently reduced.
It also affects cancer patients suffering from cancer due to weakened immune system and newborns for their immaturity.
Vaginitis and vulvovaginitis by Candidiasis
It is relatively common. It is characterized clinically by:
- Very intense vulvar and vaginal burns, especially when urinating.
- Congested and very red aspect of the genital mucosa.
- Appearance of whitish patches on red mucous membrane.
- Vaginal secretions whitish and dense, with lumps. Described as “with a cheese-like appearance”.
- Vaginal secretions and candidose.

Balanitis by Candida
It is less common than vaginitis. It is normally associated with diabetes, in uncircumcised individuals or whose partner has already suffered from Candidiasis.
On the glans or foreskin of the reddish lesions appear to the eroded appearance as well as superficial pustules, normally painful. They can be accompanied by burning sensations that increase when urinating.
Cutaneous Candidiasis
It appears basically in the skin folds and in areas where the tightly fitting clothes occlude the skin. This is due to the fact that in both cases, hot and relatively humid zones are created.
It presents with a reddish eruption which causes intense itching and discomfort. It is located mainly on the buttocks, under the breasts, in the genitals and other areas of the skin. In addition, hair follicles can sometimes become infected and small pimples appear.
Diaper dermatitis is relatively common in infants; this one is superinfect by Candida, sharpening the symptoms of the first.
Polyendocrinopathy autoimmune type 1
It is a very rare genetic disease due to a mutation in the AIRE gene. The disease starts from childhood with repeated, oral and nail-like candidiasis, without any apparent reason.
Later a malfunction of autoimmune origin appears in several glands. Then there are frames of hypoparatyroidism, adrenal insufficiency and Addison’s disease.
Deep Candidiasis
Oesophagitis by Candida
It is typical in immunosuppressive patients. It occurs very frequently in patients with HIV or lymphoma, and less often during corticosteroid treatments. The symptoms are very particular:
- Retrosternal burning
- Difficulty digesting (dysphagia)
- heartburn
In addition, whitish pseudomembranes appear throughout the esophagic mucosa.
Invasive candidiasis
In these cases the fungus passes into the bloodstream and can affect almost any organ. It appears in patients with severe immunosuppression (poorly controlled and terminally ill).
This is a very bad case, poorly predicted in the majority of cases.
Diagnosis
The diagnosis is made by obtaining and analyzing the area affected. They are taken by a smear on the affected area . Then, the samples will be analyzed under a microscope.
Prevention and treatment

It is important to maintain good personal hygiene. After the shower, dry the skin folds well and take care of the genital area. In the case of pregnant women it is also advisable to consume bioactive yogurt which promotes the maintenance of vaginal acidity.
intimate hygiene and candidiasis
Treatment is different depending on the type of fungus. The most common is the typical treatment with Clotrimazole (see treatment for candidiasis).